Hip Dysplasia Treatment Options
What is hip dysplasia?
Hip dysplasia is a common musculoskeletal disorder characterized by an abnormal development of the hip joint, leading to instability, pain, and functional impairment. It affects individuals of all ages, from infants to adults, and if left untreated, it can result in debilitating arthritis and decreased quality of life. The treatment of hip dysplasia depends on various factors, including the patient’s age, severity of symptoms, and degree of joint damage. The overarching goals of treatment are to alleviate pain, improve joint stability, and prevent the progression of osteoarthritis. The management strategies for hip dysplasia encompass both conservative and surgical approaches.
What nonoperative options are available?
Nonoperative management of hip dysplasia is aimed at alleviating hip pain, restoring hip functioning, and avoiding the long-term joint degeneration sequalae of hip dysplasia.
- Lifestyle Modifications: Patients are advised to avoid activities that exacerbate hip pain, such as high-impact sports or prolonged standing.
- Physical Therapy: Targeted exercises aim to strengthen the muscles surrounding the hip joint, enhance flexibility, and improve overall joint function.
- Orthotic Devices: The use of orthotic devices, such as braces or shoe inserts, may help stabilize the hip joint and alleviate symptoms, particularly in children with developmental dysplasia of the hip (DDH).
- Pharmacological Interventions: Nonsteroidal anti-inflammatory drugs (NSAIDs) or intra-articular corticosteroid injections may be prescribed to manage pain and inflammation.
What operative options are available?
Operative management of hip dysplasia is reserved for patients who fail to improve with nonoperative measures. A variety of operative options are available. Dr. Shane J. Nho helps guide patients to the correct operative solution for them.
Hip Arthroscopy
Hip arthroscopy has emerged as a minimally invasive surgical option for managing hip dysplasia, especially in cases associated with labral tears, femoroacetabular impingement (FAI), or loose bodies within the joint. During hip arthroscopy, small incisions are made around the hip joint, and a specialized camera (arthroscope) is inserted to visualize the intra-articular structures. Surgical instruments are then used to address labral pathology, remove impinging bone, and address any other intra-articular abnormalities contributing to hip pain and dysfunction. Furthermore, capsular tightening or plication may be pursued to aid in further stabilizing the hip joint. While hip arthroscopy alone does not correct underlying dysplastic bony anatomy, it can provide symptomatic relief and improve joint function in selected cases.
Periacetabular Osteotomy (PAO)
Periacetabular osteotomy is a surgical procedure designed to reorient the acetabulum, thereby improving coverage of the femoral head and enhancing joint stability. During PAO, the acetabulum is mobilized from the pelvic bone and repositioned using specialized osteotomy techniques. This allows for better distribution of joint forces and may help prevent the progression of osteoarthritis. PAO is particularly indicated in young adults with symptomatic hip dysplasia who wish to preserve their native hip joint and delay or avoid the need for total hip replacement.
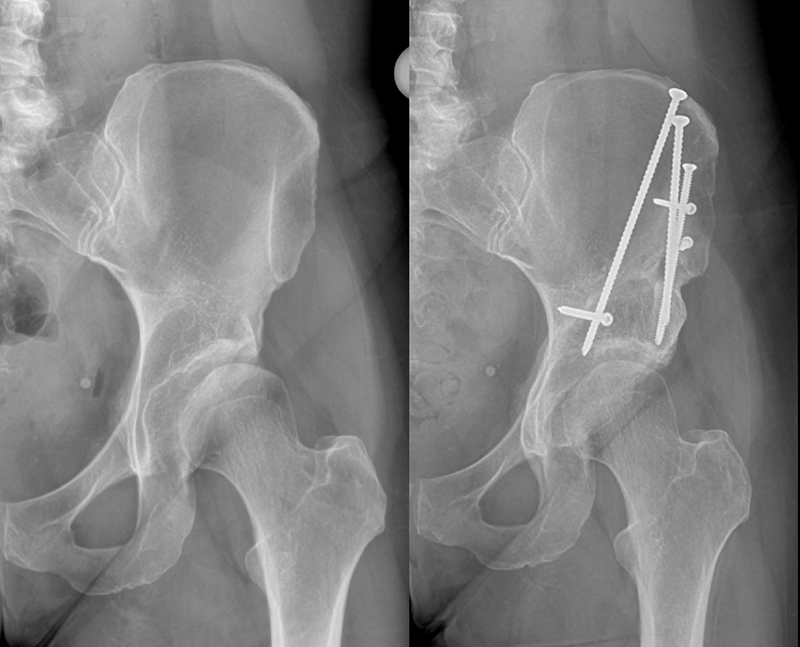
Staged Hip Arthroscopy and PAO
Hip arthroscopy followed by PAO a couple weeks later may be indicated for select patients. Use of first hip arthroscopy for the repair of labral tears, correction of concomitant FAI deformity, and capsular tightening or plication is pursued prior to the surgical repositioning of the acetabulum through the PAO. This staged procedure offers the advantages of both procedures in the correct setting.
Total Hip Arthroplasty (THA)
Total hip replacement is reserved for patients with severe hip dysplasia who have advanced osteoarthritis, significant joint deformity, or failed previous surgical interventions. During THR, the diseased hip joint is replaced with prosthetic components, including a metal acetabular cup and a ceramic or metal femoral head. Total hip replacement effectively relieves pain, restores joint function, and improves quality of life in patients with end-stage hip dysplasia. Modern advancements in implant design and surgical techniques have led to excellent long-term outcomes following total hip replacement in appropriately selected patients.
What does postoperative rehabilitation entail?
Rehabilitation after Hip Arthroscopy and Periacetabular Osteotomy (PAO) plays a crucial role in optimizing outcomes and facilitating the return to activity for patients with hip dysplasia.
- Following hip arthroscopy, rehabilitation focuses on promoting early mobilization, restoring range of motion, and strengthening the surrounding musculature. Initially, patients may engage in gentle passive and active-assisted range of motion exercises to prevent stiffness and promote healing of the soft tissues. As pain and inflammation subside, progressive strengthening exercises targeting the hip abductors, adductors, flexors, and extensors are introduced to improve joint stability and function. Additionally, neuromuscular retraining exercises, such as balance and proprioception drills, help enhance joint proprioception and control. Physical therapists work closely with patients to gradually increase the intensity and complexity of exercises while monitoring for signs of overexertion or joint irritation.
- Following Periacetabular Osteotomy (PAO), rehabilitation is typically more extensive and may involve a longer recovery period compared to hip arthroscopy. In the early postoperative phase, weight-bearing restrictions and precautions are implemented to protect the osteotomy site and allow for proper healing. Physical therapy focuses on regaining hip range of motion, improving muscle strength and coordination, and restoring normal gait mechanics. Patients may initially use assistive devices such as crutches or a walker to offload the operated hip and facilitate safe ambulation. As healing progresses, gradual weight-bearing progression and functional activities are introduced, guided by the surgeon’s protocol and patient-specific factors.
When can I return to activity?
The timeline for return to activity varies depending on the individual patient’s progress, surgical technique, and rehabilitation protocol. Patients undergoing hip arthroscopy may begin low-impact activities such as stationary biking or swimming within a few weeks to months postoperatively, with a gradual transition to higher-impact sports or activities as tolerated. Similarly, patients undergoing PAO typically experience a gradual return to full weight-bearing and activity participation over several months, with a focus on achieving optimal hip strength, stability, and range of motion before resuming more demanding activities. Close communication between the patient, Dr. Shane J. Nho, and their physical therapist is essential to ensure a safe and successful return to desired activities while minimizing the risk of reinjury or complications.
Dr. Shane J. Nho is a board-certified fellowship trained sports medicine orthopaedic surgeon who specializes in the treatment of hip dysplasia. If you believe you are affected by hip dysplasia, schedule a consultation today with our experienced orthopaedic care team.
At a Glance
Dr. Shane Nho
- Board-certified, fellowship-trained orthopedic surgeon
- Team Physician for Chicago Bulls, White Sox, Steel
- Performs more than 700 procedures each year
- Learn more
